Join us to improve the health and well-being of women everywhere through clinical excellence, compassionate inclusive care, discovery, innovation and education.

Our team of physicians, nurses, nurse midwives (and more) is dedicated to breaking boundaries in all areas of obstetrics and gynecology research and care. We are consistently ranked among the best in the nation for our efforts in advancing the future of women’s health care worldwide. Looking ahead, we’re focused on leveraging our experience, talent, state-of-the-art technology and uniquely collaborative environment to increase our contribution to this important field.
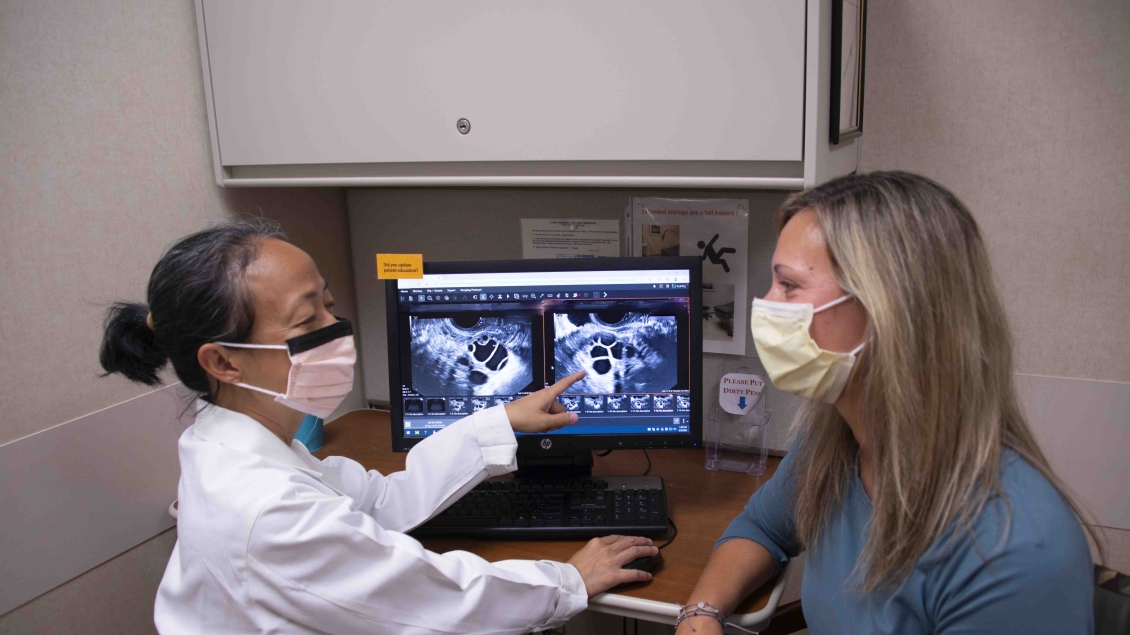
Explore our comprehensive obstetric and gynecologic care specialties.
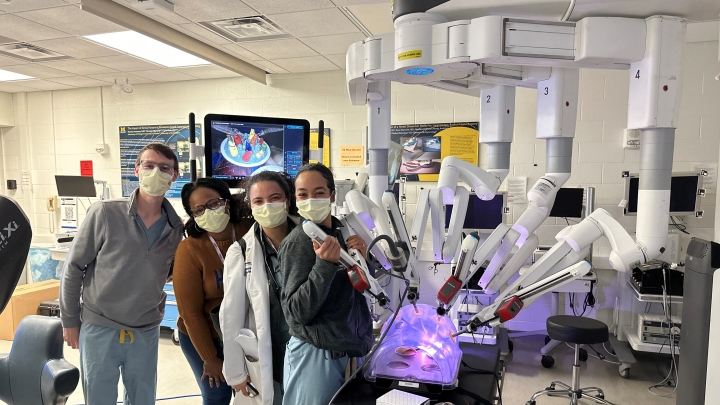
The values of diversity, equity, and inclusion are woven into everything we do, including how we care for patients, teach the next generation of physicians, and design and conduct research. We actualize our commitment to DEI by carefully examining our performance, listening to members of our community, and constantly seeking to improve.
The Department of Obstetrics and Gynecology is taking on challenges that impact women and families everywhere. Our physicians, nurses, midwives, and researchers are breaking boundaries and accelerating education and care to ensure that women have access to the treatments and resources that can change their lives.